 A dramatic case report has just been published on the extraordinarily quick recovery of a woman diagnosed with “severe and complex” PTSD and unspecified Dissociative Disorder. The author is trauma therapist Anna Gerge of Sweden, and the method was ten sessions of Infra-Low Frequency Neurofeedback, in combination with a single session of EMDR. Substantial resolution of PTSD symptoms and essentially complete resolution of dissociative events was achieved, and confirmed in four-month follow-up.
A dramatic case report has just been published on the extraordinarily quick recovery of a woman diagnosed with “severe and complex” PTSD and unspecified Dissociative Disorder. The author is trauma therapist Anna Gerge of Sweden, and the method was ten sessions of Infra-Low Frequency Neurofeedback, in combination with a single session of EMDR. Substantial resolution of PTSD symptoms and essentially complete resolution of dissociative events was achieved, and confirmed in four-month follow-up.
The client, now in her forties, was sexually abused in childhood in a shame-based culture, and she also suffered civil-war-related trauma that involved missing and murdered relatives. She suffered through an abusive relationship in adulthood. Her brother was murdered two years before therapy was initiated. Between two assessment events ten weeks apart, the one parent with whom she had a partly secure attachment died.
 The early sexual abuse by a family member was described as “massive childhood traumatization”; the abusive relationship in her adulthood was one of “severe violence;” the death of the one parent with whom the client had a viable relationship was seen as a consequence of the grief and despair related to the murder of her son. In consequence, the client was in the early stages of mourning the death of her parent as the therapy was undertaken.
The early sexual abuse by a family member was described as “massive childhood traumatization”; the abusive relationship in her adulthood was one of “severe violence;” the death of the one parent with whom the client had a viable relationship was seen as a consequence of the grief and despair related to the murder of her son. In consequence, the client was in the early stages of mourning the death of her parent as the therapy was undertaken.
Therapy consisted of ten sessions of Infra-Low Frequency (ILF) Neurofeedback utilizing Othmer protocols (Ref. 2), plus one session of EMDR. Between the second assessment and follow-up at four months, PCL-5 score improved by 83%, from 71 to 12. SCL-90-R score improved by 98%, going from 223 to 4. DES, the Dissociative Event Scale, improved by 97%, going from 62 to 2, with all of the improvement coming in the NF portion of the therapy. The DES-taxon, a subscale of the DES that is more specifically indicative of DID, declined by 100%, going from 61 to 0.1. The Symptom Rating Scale, SR, improved by 98%, going from 8.1 to 0.2. The Positive States of Mind Scale, PSOM, improved by a factor of 3.6, going from 5 to 18, with most of the improvement occurring during the NF portion.
Here the ILF neurofeedback served to calm and stabilize the nervous system to the point where even a single session of EMDR could be highly productive. In a comprehensive neurofeedback strategy, this part of the therapy would have been pursued with Alpha-Theta training. Alpha-Theta training is more scalable than the consummate clinical skills of Anna Gerge.
A brief survey of the session history reveals that the first session only lasted twenty minutes. She fell asleep easily that night, to her own surprise. The second session was 25 minutes, followed by a notable good night of sleep. A clear relaxation response was experienced at the third session, and the client was happy during the session. At the fifth session the client reported feeling a sense of calm and further improvement in sleep. Progress continued along those same lines at session six. Session seven, following on Halloween, was one of great sorrow on missing her parent, accompanied by higher levels of pain. Calmness returned with session eight, at which time a third protocol, targeting emotional regulation, was first introduced. Up to that time, the training relied on our two starting protocols, {T4-P4} and {T3-T4}, which target arousal regulation and brain stability, respectively.
Such rapid recovery in a severe case, although not routine, is by no means unprecedented. We reported such a case back in 2009, in which a formerly homeless Vietnam War veteran with a forty-year history of PTSD showed 50% improvement in his most salient PTSD symptoms over three sessions, with over 90% recovery by session 18. (Ref. 3) The sole modality employed here was ILF NF, which was then still early in its development.
Ref. 1. Gerge, A. (2020). A multifaceted case-vignette integrating neurofeedback and EMDR in the treatment of complex PTSD. European Journal of Trauma & Dissociation, 4(3), 100157
https://doi.org/10.1016/j.ejtd.2020.100157
Ref. 2. Othmer, S., & Othmer, S. F. (2009). Post-Traumatic Stress Disorder – The Neurofeedback Remedy. Biofeedback, 37(1), 24–31. http://dx.doi.org/10.5298/1081-5937-37.1.24
http://www.eeginfo.com/research/articles/PTSD-NeurofeedbackRemedy.pdf
Ref. 3. https://news.eeginfo.com/recovery-from-ptsd-a-vietnam-veteran/
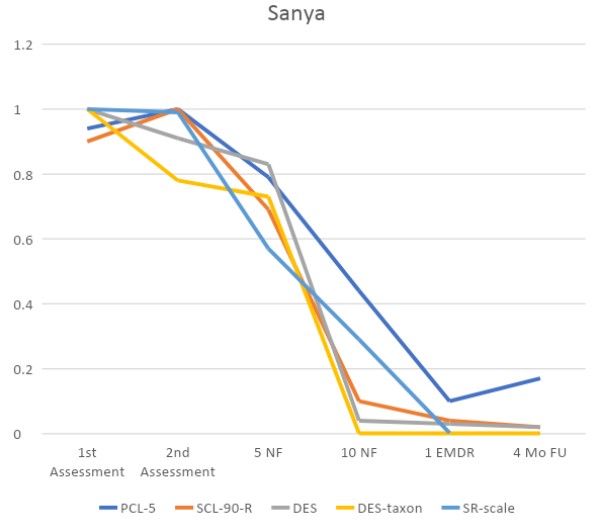
Temporal contour of symptom rating scales. PCL-5, PTSD Checklist; SCL, Symptom Checklist; DES, Dissociative Events Scale; DES-taxon, subset of DES; SR, Symptom Rating Scale. All trend lines were normalized to peak value for ease of comparison.

