The July issue of Scientific American features an article about cognitive therapy as an alternative to ADHD drugs. The work proceeds from the assumption that cognitive deficits in general, and working memory deficits in particular, are among the defining features in ADHD, and yet are only marginally addressed with stimulant medication. According to Rosemary Tannock of the Department of Psychiatry at the University of Toronto, the effect of stimulants on working memory is positive but small. Working memory deficits are thought to underlie a number of disorders beyond ADHD, and that argues for a direct approach to training working memory.
In a recent paper in the Journal of the American Academy of Child and Adolescent Psychiatry, Torkel Klingberg of the Karolinska Institute in Sweden reports that some 12 out of 20 ADHD children could no longer be diagnosed as ADHD after a mere five-week training program. Moreover, a follow-up to the $6M Multi-site study of ADHD found that after two years the behavioral treatment arm was functioning better than the medication-only arm, a reversal from the findings after only one year. Moreover, only 8% of the children in the behavioral arm added medications in the second year. Most of them continued to rely totally on the benefit they had derived from the behavioral treatment and the acquired parenting skills.
This story inspires a number of thoughts. First of all, it should be observed that the Klingberg study was apparently an outcome study, not a controlled study, and yet the results were welcomed and accepted. The problem is obvious. How does one deliver fake cognitive skills training? One does not, and the world moves on regardless. We should insist on the same liberties with neurofeedback. It is a training; it is contingent on the active involvement of the client and the clinician; it should not be attempted blindly.
Secondly, one might wonder why it is that simple techniques such as training in Digit Span should gain notice in top-ranked journals while neurofeedback is still knocking at the door. There is only one sufficient reason: neurofeedback suffers from having been discovered far too early, so now it is operating under the lingering handicap of early rejection and neglect. Any new idea that surfaces within the current ascendancy of cognitive neuroscience does not necessarily suffer the same fate. At least it is given a hearing. An ancillary reason is that training in Digit Span does not threaten the medical edifice, whereas neurofeedback does. All of this is just to say, once again, that the fault does not lie within ourselves, dear brutal critic, within our professional community, and least of all with the inadequacy of either our data or our models. Can any neurofeedback researcher imagine going to press on ADHD in 2005 with a sample of 20 and a positive outcome in only 60% of subjects? The folks at the Karolinska Institute should read Tom Rossiter.
Thirdly, let us probe further into the implications of this finding. Why should an increase in working memory have such a broad effect on ADHD? The authors might argue that the defining behaviors in ADHD could be considered as a secondary consequence of the primary deficit in working memory. Poor attention follows, and hence distractibility. I would suggest an alternative view: Good working memory is contingent on the person’s capacity for the maintenance and persistence of states, and that in turn is contingent on the brain’s capacity to sustain specific EEG rhythms for the duration of the mental process or behavioral objective. The maintenance of continuity in EEG rhythmic patterns imposes the tightest constraints on the integrity of brain function. When the brain is trained so that such constraints are met for the “observable” of working memory, then they must be adequate for the control and regulation of behavior in general. Thus any improvement in working memory capacity will have its favorable fallout for behavioral control in general, and an improvement in the temporal organization of brain activity, achieved by any means, will have its favorable fallout for working memory.
Thus it should have been no surprise that successful neurofeedback training for ADHD offers the fringe benefit of improved working memory; hence improved scores on Digit Span, Arithmetic, and Coding; and hence improved scores on the Wechsler IQ test. This has by now been convincingly shown by all neurofeedback studies that have used IQ measures, with the singular exception of the Thomas Fuchs study, where the average improvement in IQ score was a mere 4 points.
The same could be said for visuo-spatial organization. Improved organization of brain timing should have beneficial fallout for visuo-spatial functioning as well as for behavior. As it happens, neurofeedback training has its most significant effect on Picture Arrangement and Picture Completion on the Wechsler. When all is said and done, no subtest of the Wechsler remains untouched by neurofeedback.
The above makes the case for the general model of disregulation in ADHD, and for the near universal utility of training the brain in the timing and frequency domains. The generalized model must come to terms, however, with the particularity we sometimes see in the deficits of ADHD children. A generalized model would lead one to expect slippage on all of the relevant dimensions of cognitive performance and behavioral control, whereas in many cases the deficits can be quite narrowly delineated. And on the remediation side, one would then expect that neurofeedback would help fairly uniformly across the board. When we look at individual responses, however, there is considerable variability.
We may argue successfully that the generalized disregulation model is the best starting point for the discussion of neurofeedback, but matters can’t end there. The observed variability in outcomes means that we must also come to terms with the more conventional neuropsychological categories where matters appear to differentiate.
A couple of weeks ago I wrote about the recent treatment of ADHD in the Journal Biological Psychiatry. There three broad categories were identified as candidates for comprehensive models of core deficits in ADHD: 1) an executive function (EF) deficit model; 2) a cognitive-energetic (arousal deficit) model; and 3) a motivational (reward-deficit) model. The first of these has the advantage of being the most accessible to quantification; it has been the most thoroughly explored; it has the benefit of august sponsorship (Barkley); and it offers the cleanest differentiation with respect to the clinical “near neighbors” of Conduct Disorder and Oppositional-Defiant Disorder.
So I took another look at the report by Nigg et al on three different studies using a variety of Executive Function tests. The averaged results are shown in Figure 1. The Figure illustrates the number of individuals exhibiting from zero to five deficits on executive function tasks for normals and ADHD children. The criterion for deficit was functioning beyond the ninetieth percentile of the normal population. Since the data refer to 100 subjects, the numbers can be read as percentages. Remarkably, some 21 percent of ADHD children showed no executive function deficit at all. And one quarter of both groups exhibited one deficit in the five tests.
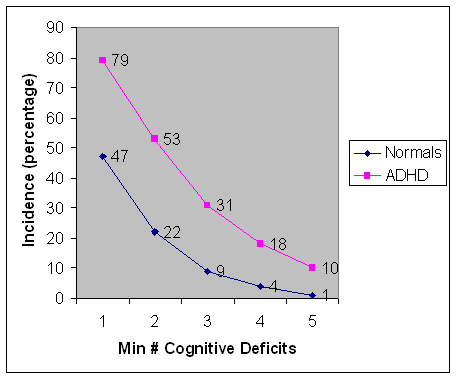
If instead one plots the cumulative score (all those scoring equal to or more than a particular number of deficits from one to five) matters are somewhat better (see Figure 2). Still, half of normals show at least one EF deficit. Improved positive predictive power (through raising the bar on the number of deficits qualifying a child as ADHD) is purchased only at the cost of diminished negative predictive power (those left out are only normals). For all the effort at characterization there seems to be only a modest benefit. Certainly this cannot be justified in support of proper diagnosis, and EF cannot be considered a defining deficit in ADHD except possibly for a subgroup (where that would be true by definition).
As already suggested previously, we need not be caught up in this dilemma at all, since it is not necessary for us to do homage at the way station of ADHD diagnosis. The ground truth is one of considerable heterogeneity in performance, even within what might come to be called the “executive function” subtype of ADHD. For us the question reduces to an operational one: must we target the executive function deficits specifically with neurofeedback, or will they all resolve with a “general self-regulation strategy.” If the latter were the case, then the general disregulation model would be supported, even in the face of the diversity of clinical presentations. But to prove the point, there is no way around our needing to assess broadly with respect to executive function deficits.
The tests at issue include the “Stop Signal Reaction Time” (SSRT) test described two weeks ago; Reaction Time Variability; the Stroop; the CPT; and the Trailmaking Test. The last of these was at the low end in terms of predictive power, so we’ll drop it from the discussion. We have prior experience with the Stroop, and found efficacy of NF in the early work with David Kaiser. Reaction Time Variability is part of the CPT. So if one were to add the “SSRT” and the Stroop to the CRT evaluation, most of the bases would be covered.
The 1991 Marks/Othmer study showed clear evidence that the neurofeedback impacted favorably on both arousal-related and motivational dimensions, as well as on emotional regulation generally. The significance of that early study was that all such results were traceable to essentially a single protocol (hence motivating the generalized self-regulation model). With the proliferation of training sites that has since occurred, and with the tailoring of the protocol to individual needs that is now possible, we may well have surmounted the high variability in outcomes found in that early work. The addition of frontal sites has improved our access to the arousal and affective dimension of ADHD. The addition of pre-frontal training has improved our impact on executive function. And the inclusion of parietal training has improved our impact on sensory processing and sensory integration issues.
Does such proliferation of protocols undermine the general disregulation model? Perhaps not. If it can be proved that with such more comprehensive tools we can achieve more uniformly successful outcomes, then one may consider the general disregulation model to be viable even in the face of the obvious heterogeneity in clinical presentation. After all, we are talking about essentially the same protocol applied at various site pairs, which apparently gives us differential access to certain parts of the regulatory networks.
But we already know that the general disregulation model is not the whole picture. It cannot accommodate specific learning disabilities, as one example. So we will just have to come to terms with both realities, both in the conceptual realm and in actual practice.
Figure 1. Distribution of Executive Function deficits for normals and ADHDs, ranging from zero to five.
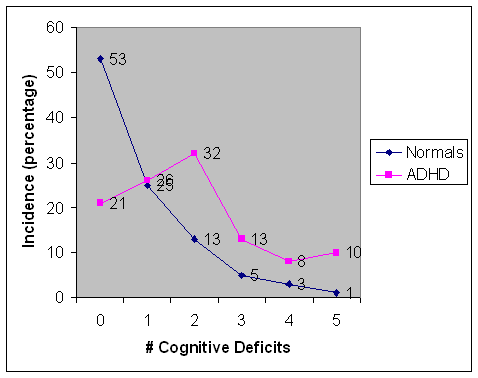
Figure 2. Partial sums of Executive Function deficits with respect to a minimum, plotted as a function of the minimum number of deficits.